The Challenge
Fertility is assumed unless proven otherwise, yet few women are taught what natural fertility actually is or how their hormonal rhythms connect to overall health — from mood to metabolism. Hormonal birth control is often prescribed by default, even preemptively. It hijacks the body’s natural communication between the brain and ovaries, masking underlying imbalances and bypassing deeper understanding.
Furthermore, while most women want to have children at some point, we rarely talk about our fertility life goals until the moment is right in front of us. We plan for our careers, finances and other life milestones — yet not our family-building timeline. Many women suppress ovulation for years with daily hormonal birth control, without ever having a conversation about what’s happening in their bodies or what their “normal” looks like. If having children is a life goal, it’s a conversation that needs to start earlier — with education, body literacy and an understanding of what fertility actually means, long before it becomes urgent.
In short, women are under-educated, under-tested and under-supported — not because we are ignored, but because the system was never designed to help us understand our own bodies. With so much conflicting (and commercialized) information, many women don’t know where to start. What should feel empowering ends up feeling incredibly intimidating.
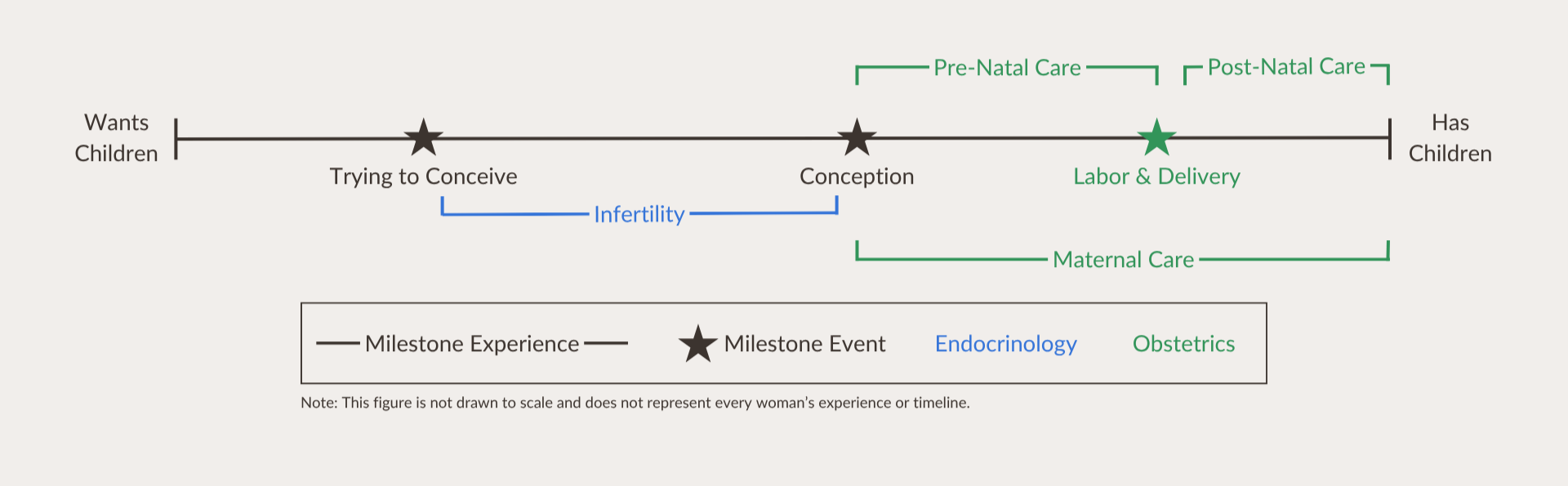
This timeline reflects a system that waits for milestones to appear instead of supporting the years that shape them.
Today’s healthcare system is not built for proactive women’s healthcare. Most providers are doing their best within a reactive model of care that prioritizes disease management over education, preparation and prevention.
Care today is limited by:
A lack of foundational education around women’s reproductive physiology
Women are not encouraged to build fertility literacy nor taught how to observe, track or interpret their cycles, leaving them disconnected from the most consistent data their body provides.
Fertility being treated as situational, not foundational
Most women are taught to think about fertility only when pregnancy becomes a goal, rather than as a lifelong indicator of hormonal, metabolic and overall health.A model that prioritizes symptom management over insight
Appointments default to suppressing symptoms or preventing pregnancy, rather than understanding and supporting ovulation, cycle health and a woman’s long-term reproductive goals.A system designed to intervene late, not support early
Meaningful conversations, deeper testing and longitudinal context are often reserved for when a woman is actively trying (and struggling) to conceive.
As a result, women are left to navigate a fragmented, confusing system on their own. They face:
Rising rates of hormone-related symptoms that are normalized or dismissed (irregular cycles, acne, hair loss, mood changes, metabolic shifts, fatigue, painful periods, etc.)
Fertility challenges that feel sudden, despite years of underlying signals
Anxiety and burnout from trying to self-educate without guidance or context
A disconnect between how they feel and what they’re told is “normal”